|
|
||||||||||||||
|
|
||||||||||||||
Your doctor has explained that you have colorectal cancer (colon or rectum) and has recommended treatment with a novel agent called Erbitux (its generic name is cetuximab). This information sheet provides a brief introduction to Erbitux and explains the common side effects you may experience. This does not mean you will definitely get them. It is also possible you may experience a side effect not mentioned here. Erbitux is usually used in conjunction with a chemotherapy agent called irinotecan (Campto) but there is emerging evidence of benefit with other drugs such as 5 Fluorouracil or Oxaliplatin. The exact combination would have been explained to you by your doctor and you should also refer to the specific information and advice sheet relating to these other drugs. What is Erbitux? Erbitux is not a chemotherapy or hormone but a class of agents known as monoclonal antibodies (Mab). It is similar to the antibodies the bodies immune system normally makes when we have a bacterial or viral infection, but in this case it has been made in a laboratory and attaches mainly to a specific target on cancer cells. These targets (called antigens) can be detected with special sensitive laboratory tests. In the case of bowel cancer, there is a protein receptor on the cell surface which is different from a normal bowel cell called Epidermal Growth Factor Receptor 1 (EGFR1). The Erbitux monoclonal antibody has been made to attach to the EGF-receptor on cancer cells. The antibody is therefore known as anti-EGFR-1 otherwise called cetuximab or its commercial name Erbitux. Preparation for Erbitux As
Mab's, like Erbitux, are treatments directed against specific targets in the
tumour, your doctor needs to find out if your tumour over expresses EGFR-1 before even considering treatment. This is usually
achieved by re-analysing a section How does Erbitux work? Monoclonal antibody therapy works in a different way than standard cancer therapy, such as chemotherapy or hormone therapies. Erbitux is believed to function in three different ways:- 1) Blocking tumour cell growth: Erbitux binds to the EGFR proteins (receptors) on the tumour cell surface. After binding it inhibits the cells ability to invade or spread to other tissues (metastasis). Erbitux also reduces the cells ability to attract the local blood vessels that are necessary to support further growth (angiogenesis). Erbitux also encourages the cancer cells to die when they have reached end their natural life cycle (like normal cells do) or have been partially damaged by chemotherapy (apoptosis). 2) Signalling of the immune system: After Erbitux has attached itself to the tumour cells it is able to recruit the bodies own immune system. Immune system cells, called natural killer (NK) cells, are attracted to the bound Erbitux and are then able to kill it in the same way as a foreign bacteria or virus. 3) Working with chemotherapy: Erbitux and chemotherapy work in different ways, but when given together, the two drugs can form a partnership (synergistic). Possible mechanisms for this are to encourage apoptosis (cell death) if the cell is partially damaged by chemotherapy. Furthermore, Erbitux is thought to prevent the cells repairing themselves again after partial chemotherapy damage. How is Erbitux administered? Erbitux cannot be taken orally as it would be destroyed by your stomach. It
is therefore infused into a vein usually over a few hours.
You’ll be given the first dose slowly, usually
over two hours. After this you’ll be given one ‘maintenance’ dose every
week, and this normally takes about an hour. The first dose takes longer than
the weekly maintenance treatments because it’s usually a larger dose, intended
to ‘kick-start’ your treatment. Occasionally, as with all protein based drugs it is possible to Are there any side effects to Erbitux? When given with chemotherapy the side effects normally relate to the chemotherapy - you should also have been given an information sheet relating to your chemotherapy. Erbitux generally does not make these worse. Erbitux does, however, have some mild side effects on its own which may occur in addition to those caused by chemotherapy. The most common of these is a feeling of tiredness or mild malaise for one to two days following each infusion. Other uncommon side effects can be broadly split into two categories:- The early effects often related to an "allergic" reaction. If they do occur, it is often while the drug is being infused or shortly afterwards . Potential side effects include:
Particularly if associated with a fast pulse and lower blood pressure these symptoms indicate an early allergic reaction. As mentioned above if these symptoms are prominent the infusion has to be slowed down or rarely discontinued. The ongoing effects may occurs over the entire period of time whilst you are receiving the treatment - usually weeks to months. These could include:-
These side effects should be discussed with your doctors and specialist nurse during one of your reviews during treatment. Sometimes patients find it easier to keep a diary of symptoms to help you remember for the consultations. Why have you been recommended Erbitux? You will already have been given some treatment for your cancer. This will usually include the chemotherapy drug irinotecan, either on its own, or in combination with the drug 5 fluorouracil (5FU). Unfortunately, by the time you are to be considered for Erbitux your disease is usually progressing again. The aim of treatment now is not to cure, but to control a specific symptom caused by the tumour. This is sometimes known as palliative treatment. It is hoped that treatment improves your quality of life; therefore the side effects from the treatment should not outweigh the benefits of shrinking the tumour. How will you know treatment
is working?
How long will you take
Erbitux? Other lifestyle questions relating to Erbitux:
Further general information Your doctors and specialist nurses are in an ideal position to give you relevant information on your disease and treatment as they know your individual circumstances. Cancerbackup has a help line (0808 800 1234) and a prize winning video available in English, Italian, Urdu, Bengali, Gujarati & Hindi explaining Radiotherapy & Chemotherapy. Cancernet.co.uk has over 500 pages describing cancer, its management, practical tips and tool which patients, their carers and their doctors have found helpful during the cancer journey. |
||||||||||||||

 of
your original tumour (from the time of your original surgery or biopsy).
Occasionally, your doctor will need a more recent tumour for analysis and
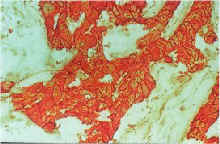
recommend a further biopsy. In either case the tumour is usually sent to a laboratory
which specialises in specific testing for antigens (targets) called
immunohistochemistry. A report will be issued by the pathologist on whether your
tumour over expresses the target and to what degree.
of
your original tumour (from the time of your original surgery or biopsy).
Occasionally, your doctor will need a more recent tumour for analysis and
recommend a further biopsy. In either case the tumour is usually sent to a laboratory
which specialises in specific testing for antigens (targets) called
immunohistochemistry. A report will be issued by the pathologist on whether your
tumour over expresses the target and to what degree.  get
an allergic reaction. The nurses will therefore be checking how you are
feeling and measuring your breathing, pulse and blood pressure regularly. Sometimes, in
response to mild reaction, it may have to be slowed down over several hours.
Rarely if the allergic reaction is prominent it has to be stopped altogether. To avoid a mild reaction often paracetamol and an antihistamine
are given before the infusion.
get
an allergic reaction. The nurses will therefore be checking how you are
feeling and measuring your breathing, pulse and blood pressure regularly. Sometimes, in
response to mild reaction, it may have to be slowed down over several hours.
Rarely if the allergic reaction is prominent it has to be stopped altogether. To avoid a mild reaction often paracetamol and an antihistamine
are given before the infusion.