For specific advise, risks & side effects to different parts of the
body click on the headings.
 RADIOTHERAPY is the use of high energy x-rays to treat patients with malignant disease.
Radiotherapy beams can be directed very accurately to any area of the body using highly
sophisticated machines. The most commonly used of these are called a linear accelerators,
with other machines called orthovoltage or superficial depending on the energy of
the X-rays required. It is also possible to deliver radiotherapy to small volumes of the
body using radioactive wires, which produce gamma rays. RADIOTHERAPY is the use of high energy x-rays to treat patients with malignant disease.
Radiotherapy beams can be directed very accurately to any area of the body using highly
sophisticated machines. The most commonly used of these are called a linear accelerators,
with other machines called orthovoltage or superficial depending on the energy of
the X-rays required. It is also possible to deliver radiotherapy to small volumes of the
body using radioactive wires, which produce gamma rays.
Because the equipment necessary to administer radiotherapy is expensive, and requires a
lot of space and specially trained staff, radiotherapy departments tend to be found in the
larger regional hospitals or cancer centres. Therefore if you do require radiotherapy you
probably have to do a lot of traveling each day.
TYPES OF RADIOTHERAPY Radiotherapy is
broadly divided into two main categories : i.e. palliative or radical. It should have been
explained which category applies to you.
Palliative means that radiotherapy is given to relieve local symptoms from a
tumour, for example to lessen pain, or stop bleeding, or to prevent damage to neighbouring
structures such as nerves. It is usually given over a short period of time, either on one
day or one or two weeks. In radical cases the aim is curative so a higher dose of
radiotherapy is given aiming to completely eradicate the tumour. This has to be spread
over a longer period, often four to six weeks, to allow your normal cells to repair.
 In either case patients' first
appointment at the radiotherapy centre will be a planning session. On arrival in the
department patients should report to the reception desk, show them their appointment card,
and will directed to the simulator. The simulator is a direct mock-up of an actual therapy
machine, but the x-rays produced are only for pictures. This helps the doctor decide the
exact area within the body that needs treatment. In some cases, patients are taken from
the simulator to the CT scanner. These scans are required to plan the radiotherapy of some
areas of the body. For patients receiving radiotherapy to the head or neck it may be
directed to the mould room where a plastercast impression is taken. - see sheet having a
mould In either case patients' first
appointment at the radiotherapy centre will be a planning session. On arrival in the
department patients should report to the reception desk, show them their appointment card,
and will directed to the simulator. The simulator is a direct mock-up of an actual therapy
machine, but the x-rays produced are only for pictures. This helps the doctor decide the
exact area within the body that needs treatment. In some cases, patients are taken from
the simulator to the CT scanner. These scans are required to plan the radiotherapy of some
areas of the body. For patients receiving radiotherapy to the head or neck it may be
directed to the mould room where a plastercast impression is taken. - see sheet having a
mould
During your visits to the radiotherapy centre you
will encounter members of staff called radiographers. These are people who operate the
machines to plan and give you your treatment. They work closely with the doctors and other
people within the department. They can give you help and advice about any aspect of your
treatment, and don't be embarrassed to ask them anything you are concerned or anxious
about.
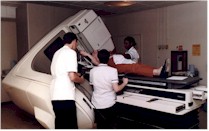 During this planning stage very
accurate measurements will be taken of the body, and it does require the patient to be
lying on a fairly hard couch, which may be slightly uncomfortable. In some cases a small
tattoo about the size of a pinhead is made, giving a permanent record of the measurements.
This is probably the longest time patients have to lie on a couch. During this planning stage very
accurate measurements will be taken of the body, and it does require the patient to be
lying on a fairly hard couch, which may be slightly uncomfortable. In some cases a small
tattoo about the size of a pinhead is made, giving a permanent record of the measurements.
This is probably the longest time patients have to lie on a couch.
Once all the measurements are taken, the rest of
the treatment planning will be behind the scenes with the aid of a physicist who is a
highly trained specialist in the subject of radiation. They assists the oncologist in
deciding the best way of delivering the amount of radiotherapy needed. Only when the
radiographers, physicist, and doctors are one hundred percent confident with your planned
treatment will patients proceed to treatment.
The treatment machine looks like the simulator,
but it is a lot bigger. Patients are not required to do anything that they've not already
done in the simulator. Treatment usually lasts one or two minutes, and while the machine
is on they usually do not have any sensation. Even though the radiographers are not in the
room while they are being treated, they are being watched at all times on a video camera.
There is also an intercom, which is left on so they can hear as well as see you
constantly. If patients feel any distress during treatment, the machine can be turned off
and the radiographers will be at their side within seconds.
 Before treatment you will be
asked to sign a consent form. The main object of this form is to clarify that patients
fully understand the treatment and are aware of any potential side effects. The risk of
side effects do depend on whether you having treatment to the breast alone or the breast
and armpit. These side effects are broadly split into early effects, which can come on
during or shortly after radiotherapy but are temporary, and late effects which can be long
term. Your oncologists will have carefully taken these into account when considering the
benefits of treatment and will inform you of the side effects you are most likely to get.
Let us now describe some of these side effects but it must be stressed that what follows
is a general overview of treatment - you may well not experience any of these effects and
it is possible you may experience others not mentioned here. Before treatment you will be
asked to sign a consent form. The main object of this form is to clarify that patients
fully understand the treatment and are aware of any potential side effects. The risk of
side effects do depend on whether you having treatment to the breast alone or the breast
and armpit. These side effects are broadly split into early effects, which can come on
during or shortly after radiotherapy but are temporary, and late effects which can be long
term. Your oncologists will have carefully taken these into account when considering the
benefits of treatment and will inform you of the side effects you are most likely to get.
Let us now describe some of these side effects but it must be stressed that what follows
is a general overview of treatment - you may well not experience any of these effects and
it is possible you may experience others not mentioned here.
The side effects of radiotherapy can
be broadly split into two categories. Firstly, the early or acute side effects. These come
on during or shortly after treatment, and depend on the size and area of the body being
treated. Your abdomen, for example, is very sensitive to radiotherapy and it is common to
suffer from nausea in this situation. This nausea can come on one or two hours after
treatment. If a large area of your abdomen is being treated, then anti-sickness tablets
are best prescribed before your treatment.
During radiotherapy your skin may get red and
itchy, similar to sunburn. Your radiographers will be looking for these reactions, but you
should let them know as soon as you feel soreness. Do not apply creams or dressings,
unless recommended by your radiographer or oncologist. Avoid sun, excessive washing, and
rubbing on these areas. Each department will have its own skin care policy, which will be
available to you.
If the ovaries in women, or the testes in men,
are being irradiated, there will be a risk of infertility and reduced hormone output which
should have been discussed with you in advance. On no account must a female patient be
pregnant, but there is no risk of harming any babies or pregnant women if you meet them
during your radiotherapy course or afterwards.
Radiotherapy to your mouth and throat will cause
some soreness (otherwise called mucositis). This usually starts halfway through your
treatment, and is at its worst towards the end of treatment, but can persist for some time
afterwards. It is important to keep your mouth clean, with regular soft toothbrushing,
dental floss, and mouthwashing. Once mucositis has started, treatment to prevent secondary
thrush infection is often given. It is also important to maintain a good nutrition, and
avoid smoking and alcohol.
With radiotherapy you will lose hair within the
treatment area. It usually begins to fall out after two or three weeks. Most hair loss is
temporary, but can be permanent in some cases. There are many other acute side effects
which have not been mentioned here, but these should have been explained to you before the
start of treatment.
Late side effects are those which can develop
months or even years after the end of radiotherapy. These are the ones your oncologist
worries about most. The type of side effect will obviously depend upon which area you are
having irradiated. For example, if your salivary glands are irradiated, you will get
dryness of the mouth which can last several months after treatment and may be permanent.
This side effect in particular should have been discussed with you before starting
treatment. Other late side effects are rare, but can cause considerable distress. These
include :-
- thickening of the skin and underlying structures
- damage to nerves
- damage to the bowel or waterworks.
- damage to the heart and lungs.
- even rarer, a secondary malignancy may be induced.
Your oncologist will have taken the risks of
these late side effects into account when deciding on your treatment strategy. In any
case, the risk is usually no more than one to five percent. These risks should have been
discussed with you during your consent consultation. For more specific information
on the various sites of the body refer to the adjacent list.
|