HIFU is a treatment designed to treat localized prostate cancer using high intensity focused ultrasound (HIFU). A rectal probe generates high intensity ultrasound waves which travel through the rectal wall and are focused in the prostate. This focusing produces intense heat and provokes the destruction of the tissue inside the targeted zone with minimal effect to surrounding tissues. The treatment typically takes 3 hours to perform, usually under a under general aesthetic. The technique is very new in the field of prostate cancer treatments and is still under research with little long term data to verify its effectiveness, However, for some patients especially with recurrent localised prostate cancer following radiotherapy it may offer use second line option.
The initial work in devising a machine that could focus high intensity ultrasound waves at the prostate began in the late 1980s following the development of transrectal ultrasound probes. Much of the early research was carried out in France and the device received a CE mark approximately ten years later. Whilst further studies have been requested from America, to demonstrate the effectiveness of the device before it receives FDA approval, many patients have already been treated in Europe.
The HIFU device consists of a number of components
- A table for the patient to lie on during the treatment.
- A ultrasound imaging system, which allows the visualization of the prostate by the urologist.
- A transrectal devise consisting of the imaging probe and the treatment transducer, which emits the focused ultrasound. These two elements are placed in a latex balloon filled with cooled liquid.
- A computer which controls and aims the high intensity beam according to the treatment plan established by the urologist.
There are a number of devices connected to the equipment to ensure the patient’s safety and optimise the treatment:
- Continuous control of the treatment probe’s position in relation to the rectal wall to avoid damage to the rectum.
- A patient movement detector to ensure the patients lies still and the prostate stays in target.
- Constant monitoring of the rectal temperature to avoid heating and damaging to the rectum.
- Constant control of the power delivered to the patient avoiding surges that may cause damage to surrounding structures.
Preparation
The patient may be hospitalized the evening before the treatment. The patient is given an enema for colorectal preparation approximately two hours before treatment.
The Procedure
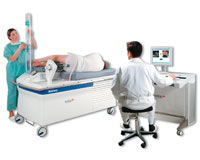
The treatment is performed under anesthesia. The treatment is executed with the patient lying in a right lateral position. Strict immobility is necessary during the treatment, which can last at least 3 hours, hence the appeal of a general anaesthetic.
A probe is placed in the rectum. This probe has a dual function, to provide both conventional ultrasound images of the prostate and well as emitting the high intensity ultrasound waves that will destroy the gland.
Initially the shape and size of the prostate are calculated and processed as the target area to be treated. As cancerous prostate tissue typically has the same appearance on ultrasound as normal benign tissue, it is not possible to accurately treat just the cancerous parts of the gland. With the intention to cure the patient of their disease, the entire prostate gland needs to be targeted and treated. From studies in patients who have undergone a radical prostatectomy, it is clear that there are commonly seven or more separate regions within the prostate gland where the cancerous tissue can be identified.
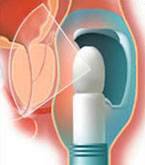
At the point where the beam of high intensity convergent ultrasound is focused (focal point) the rapid and intense absorption of the ultrasound energy creates a sudden elevation of the temperature to 100°C which destroys the cells located in the targeted zone.
The targeted zone destroyed by each pulse is oval-shaped and measures up to 24 mm in height by less than 2 mm in diameter. By repeating the pulses, and moving the focal point between each pulse, it is possible to destroy the prostate gland. Little damage occurs to the rectal wall by these pulses as the beam is not focused on this tissue.
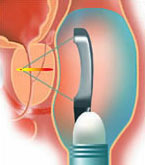
The treatment duration varies according to prostate volume and may take approximately 3 hours.
Swelling of the prostate appears immediately after the treatment due to the effective burning process of the gland. This swelling or oedema compresses the urethra and can make it difficult or impossible to pass urine initially. A temporary urinary catheter is inserted into the bladder, either through the urethra (water pipe) or through the lower abdomen (supra pubic). This allows the elimination of urine until the oedema recedes which takes generally from 3 to 8 days.
Sometimes for larger prostate glands, as well as to help reduce the need for prolonged post treatment catheterization, a “mini” transurethral resection of the prostate or TURP can be done before or immediately after the treatment with HIFU (during the same anesthesia). This procedure removes the central, obstructing portion of the prostate and is most commonly performed in men with benignly enlarged glands to improve their urinary symptoms.
Such a dual procedure is mainly performed with HIFU in patients presenting signs of prostatic obstruction (weak urinary stream, frequent nocturnal urination, residual urine volume in the bladder). Naturally combining treatments can increase the post operative complications. In particular a TURP will usually affect the ejaculatory function of a patient, causing the ejaculate to enter the bladder at the point of orgasm rather than being produced from the penis. The ability to obtain an erection can also occasionally be affected as well. For more information on transurethral resection of the prostate please read “A Patient’s Guide to a TURP” which should be available at your hospital or may be viewed and downloaded from the internet at www.prostatecancercentre.com.
After the procedure
Patients are normally able to eat and drink the evening of the treatment day, and the urinary catheter is generally removed 3 or 4 days after the session. Discharge from hospital usually takes place the day after the urinary catheter removal, once the patients is reliably able to empty their bladder. Occasionally patients can go home with a catheter in place, to return for its removal at a later date.
A prophylactic antibiotic, such as ciprofloxacin, may be prescribed for the following few weeks to prevent the occurrence of a urinary infection
During this period, you might feel some discomfort, mild bleeding in the beginning of passing urine, frequent and sometimes urgent urination and urine leakage or incontinence with exertion. Over the next few weeks necrotic debris from the prostate will be passed in the urine. If debris or blood are seen in the urine it is important to maintain a high fluid in take. Caffeinated drinks should be avoided as they may increase urinary frequency or urgency. Infections with fever are rare but possible, and if a patient feels generally unwell they should contact their physician immediately for an appropriate antibiotic.
Follow-up Visits after the Treatment
Three to six months after the treatment, control biopsies may be performed under local anesthesia: if they are negative, regular checking of PSA every three months for the first year then six monthly is sufficient.
If a residual cancerous zone is detected on biopsy (about 10% of the cases), a second treatment can be conducted 6 months after the initial session or an alternative therapy may be considered.
If the biopsies are negative but the PSA rises, imaging is required to identify whether the prostate cancer has spread to the pelvic lymph glands or the bones. If so, hormone therapy may be the next treatment to consider. If the tumour appears still confined to the prostate, external beam radiotherapy or prostate cryotherapy may be treatment options, if they have not been previously used. However as many urologists feel that HIFU should only be used in patients who have failed an initial first line therapy such as prostate brachytherapy or radiotherapy the individual treatment history of the patient will affect the options available.
For more information on external beam radiotherapy, prostate cryotherapy of brachytherapy please read “A Patient’s Guide to a Prostate Cancer”, “A Patient’s Guide to a Cryotherapy”, “A Patient’s Guide to a Prostate Brachytherapy” which should all be available at your hospital or may be viewed and downloaded from the internet at www.prostatecancercentre.com.
The main side effects with HIFU when used to cure patients with prostate cancer are as follows:
- Difficulty passing urine which requires all patients to be initially catheterized following the treatment before the swollen prostate reduces in size, which may take a week or more.
- Urinary frequency, urgency and burning that may be aggravated by drinking caffeinated drinks post procedure.
- Rectal burning and bleeding which is most common in patients treated with multiple HIFU sessions.
- Urinary leakage or incontinence occurring with physical exertion is seen in one in twenty patients but will often settle in time with pelvic floor exercises.
- Impotence, the inability to get and erection, which is a common side effect in such men occurring in more than 70% as the tiny nerves supplying the erectile tissues of the penis lie on the outer surface of the prostate gland and may be damaged during treatment.
- When a TURP is performed in conjunction with HIFU, patients will normal experience a retrograde or internal ejaculation at the time of orgasm, as the part of the prostate that is removed causes the ejaculate to be released into the bladder rather than being produced from the penis. This effect is usually permanent.
Due to the lack of long term clinical data regarding the effectiveness of HIFU in the treatment of prostate cancer many urologists believe that HIFU should not be used as a first line option. Indeed, due to this lack of data the treatment has not yet received a license to be offered in the USA. Currently proven effectiveness of existing treatments such as radical prostatectomy and brachytherapy appear to offer higher chances of long term cure with better side effect profiles. However, clinical trials have begun in Europe which will hopefully demonstrate the value of HIFU.
HIFU is only an option for localized prostate cancer (stage 1 or 2) as little of the surrounding tissue is treated. It may be best reserved to patients who have already been treated by either radiotherapy or cryotherapy in whom the cancer has recurred within the gland.
Researchers are investigating whether treating just part of the prostate rather than the whole gland may be effective in suppressing the disease and PSA, even though it is known that the cancer is normally multifocal and spread through the prostate at the time of diagnosis. The thought behind such a treatment strategy is that multiple further treatments in the future can be given if and when required. Such an untested approach to the treatment of prostate cancer should be regarded with caution as the risk of significant side effects increases with multiple HIFU sessions and the chance of the cancer spreading from the prostate between treatments remains a real possibility.
HIFU is a novel therapy using complex computer assisted equipment to treat prostate cancer. It usually required a 2-3 hour anaesthetic to perform and patients are catheterised for a short while after treatment. Whilst the science and concept is inviting, detailed studies have yet to show its long term effectiveness, which is critical in assessing a prostate cancer treatment, and the side effects associated with this treatment can be significant.